
Quick Answer About Pituitary Gland Injuries:
The pituitary gland is a small but powerful gland at the base of your brain that controls nearly every hormone in your body. A truck crash, car accident, or serious fall can damage it — disrupting hormones that regulate your energy, mood, weight, memory, and more. This injury is frequently missed by emergency doctors and dismissed by insurance companies. But it is real, diagnosable, and fully compensable in a personal injury case. Doctors may call it post-traumatic hypopituitarism or PTHP — but what matters is that your body stopped working the way it used to, and pituitary gland injury from trauma is why.
For a legal consultation with a personal injury lawyer, call (434) 817-3100
“The Scans Were Normal. So Why Do I Feel Like This?”
Six months after your truck accident, you are a different person.
You sleep nine hours and wake up exhausted. You’ve gained fifteen pounds without changing what you eat. You have no interest in things that used to matter to you. Perhaps you feel cold when everyone else is comfortable. You forget simple things.
Your doctor ran bloodwork. Everything came back “normal.” The insurance company is calling your symptoms stress or anxiety. Your family is starting to wonder if you’re exaggerating.
You’re not.
What you may have is pituitary gland damage — a hormonal injury caused by the physical forces of a serious crash. It’s one of the most underdiagnosed consequences of truck accidents, car wrecks, and catastrophic falls. And because it doesn’t show up on a standard CT scan or basic blood panel, it gets missed — sometimes permanently.
This article explains what the pituitary gland does, how a crash damages it, what symptoms to watch for, and what you need to do to protect your health and your legal claim.
At MartinWren, P.C., we represent victims of these invisible injuries in Charlottesville, Richmond, and across Virginia.
What Is the Pituitary Gland — And Why Does It Matter?
Your pituitary gland is roughly the size of a pea. It sits at the base of your brain, tucked into a small bony pocket in the skull. Despite its size, it runs nearly everything in your body that you take for granted — your energy, your mood, your metabolism, your ability to handle stress, your reproductive health.
Doctors call it the “master gland” because it controls other glands throughout your body. When it receives signals from the brain, it releases hormones that tell your thyroid, adrenal glands, and reproductive organs what to do.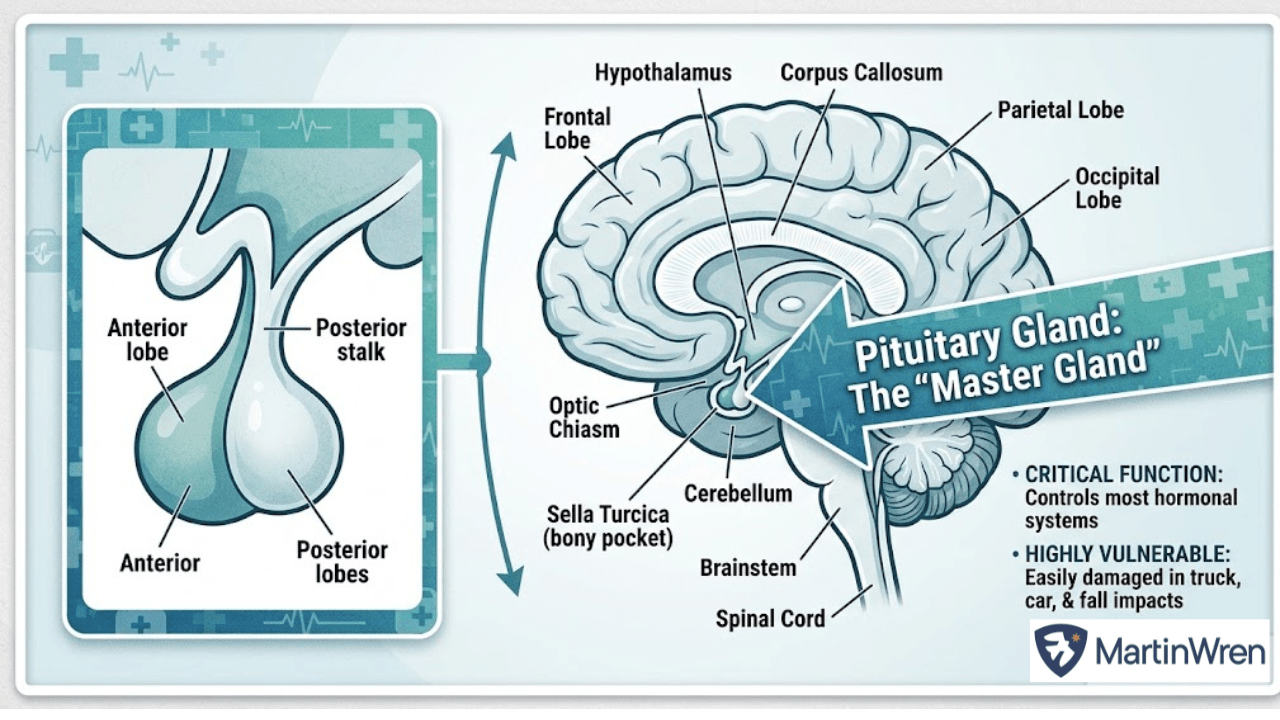
Here’s what the pituitary gland controls:
- Energy and metabolism — through thyroid-stimulating hormone (TSH), which drives your thyroid
- Stress response — through a hormone called ACTH, which tells your adrenal glands to produce cortisol
- Body composition — through growth hormone (GH), which regulates muscle, fat, and how your body uses energy
- Reproductive function — through LH and FSH, which control testosterone, estrogen, and menstrual cycles
- Fluid balance — through antidiuretic hormone (ADH)
- Emotional well-being — indirectly, through nearly all of the above
When the pituitary gland is damaged, any of these systems can break down. Often several break down at once. The result is a person who looks fine on the outside but feels profoundly wrong on the inside — and can’t get anyone to explain why.
The pituitary gland connects to the brain through a thin stalk — sometimes called the pituitary stalk or, in medical terms, the infundibulum. It also has a delicate blood supply through small vessels called the hypophyseal arteries. Both the stalk and those vessels are vulnerable in a violent crash.
How Does a Crash Damage the Pituitary Gland?
The pituitary gland is not well-armored. That thin stalk and fragile blood supply make it one of the most vulnerable structures in the brain during a high-speed collision. When traumatic forces of an auto collision, fall, or assault occur, it is possible that the stalk and its blood supply can be damaged.
Here’s what happens at the moment of impact:
The blood supply gets cut off.
The small vessels feeding the pituitary gland can rupture or go into spasm during violent acceleration and deceleration. When blood flow is interrupted — even briefly — pituitary tissue can die. Doctors call this pituitary infarction. Dead tissue means lost function.
The stalk gets stretched or torn.
When the brain whips inside the skull — forward, backward, or rotationally — that thin stalk connecting the pituitary to the rest of the brain can be stretched or severed. This cuts the hormonal communication line between the brain and the gland.
The surrounding brain tissue swells.
After a traumatic brain injury, swelling can compress the pituitary gland and its blood supply, adding another layer of damage on top of the initial impact injury.
This is why truck crashes are especially dangerous.
A fully loaded tractor-trailer can weigh up to 80,000 pounds. When it strikes a passenger vehicle, the forces involved — violent deceleration, rotation, side impact — are far beyond what the human body is built to absorb. Rear-end crashes at highway speed, underride collisions, T-bone impacts, and rollovers all generate the kind of forces that can damage the pituitary gland’s fragile anatomy. Truck accidents are much different than car accidents.
Car accidents at significant speed carry real risk as well — particularly head-on collisions and high-speed T-bone impacts. And serious falls — from heights, on construction sites, or slip-and-fall accidents involving head impact — can generate enough force to the base of the skull to cause pituitary damage. Any crash or fall that involved a head injury should raise the question of whether the pituitary was affected.
Pituitary Gland Damage vs. Traumatic Brain Injury: What’s the Difference?
This is a question worth addressing directly, because the two injuries frequently occur together — and are frequently confused.
A traumatic brain injury (TBI) is damage to the brain tissue itself — the neurons, the white matter tracts, the cortex. TBI affects how the brain processes information, controls movement, manages memory, and regulates behavior. Symptoms include cognitive problems, headaches, balance issues, and personality changes. Visit our complete guide to traumatic brain injury claims in Virginia for more information.
Pituitary gland damage is different. It is an injury to the hormone-producing gland at the base of the brain. It affects the body’s chemical messaging system — not the brain’s circuitry directly. Symptoms are hormonal: fatigue, weight gain, low libido, cold sensitivity, mood changes, and loss of drive.
Here’s why it matters that they’re different:
They require different tests.
TBI is evaluated with CT scans, MRI, and neuropsychological testing. Pituitary damage is evaluated with hormone blood panels, stimulation tests, and a specialized pituitary MRI — which is a different study than a standard brain MRI.
One can be missed while the other is found.
A patient can receive a full TBI workup and still have undiagnosed pituitary damage — because no one ordered pituitary-specific testing.
They produce overlapping but distinct symptoms.
Both TBI and pituitary damage can cause fatigue, cognitive slowing, and mood changes. But pituitary damage also causes specific hormonal symptoms — weight gain, sexual dysfunction, cold intolerance, menstrual irregularity — that TBI alone typically does not.
Both can exist in the same patient at the same time.
In a serious truck crash, a victim may have a TBI and pituitary gland damage. Each injury has its own damages. Each needs its own documentation.
The bottom line: if a crash caused a head injury, the treating physicians should be evaluating for both.
Click to contact personal injury lawyers today
What are Symptoms of Pituitary Gland Damage?
The symptoms of pituitary damage are easy to dismiss. They don’t feel like a crash injury. They feel like something vague and wrong that no one can explain. Symptoms range from weight fluctuations to emotional fragility, cognitive fog to headaches.
The most common symptoms include:
- Crushing fatigue that sleep doesn’t fix
- Unexplained weight gain — especially around the midsection — without changes in diet
- Depression, emotional flatness, or loss of motivation — feeling like a dimmer switch was turned down
- Brain fog — difficulty concentrating, slow thinking, trouble finding words
- Memory problems — forgetting things you would never have forgotten before
- Cold intolerance — feeling cold when others are comfortable
- Low libido or sexual dysfunction
- In men: loss of muscle mass, erectile dysfunction, reduced body hair
- In women: irregular or absent menstrual cycles
- Low blood pressure or dizziness when standing up
- Headaches
- Increased body fat, decreased muscle tone — even without weight gain
These symptoms often appear gradually — weeks or months after the crash. By the time they’re fully apparent, the connection to the accident feels less obvious.
The most important thing to understand: Standard emergency bloodwork does not test for pituitary function. If your doctor ran a basic metabolic panel after your crash and said everything was “normal,” that test was not looking for this injury. Normal labs do not rule out pituitary damage.
How Is Pituitary Gland Damage Diagnosed?
Diagnosing pituitary damage requires a physician who is specifically looking for it — typically an endocrinologist or neuro-endocrinologist. An endocrinologist or neuro-endocrinologist will perform a number of tests and even imaging to evaluate whether pituitary gland damage occurred as a result of trauma. The tests and processes used include the following:
Step 1: Hormone blood panel.
This includes IGF-1 (a marker for growth hormone activity), cortisol, TSH, free T4, and reproductive hormones — testosterone in men, estradiol in women. These must be drawn under the right conditions, because hormone levels fluctuate by time of day and other factors.
Step 2: Stimulation testing.
Some hormonal deficiencies don’t show on baseline blood draws. The glucagon stimulation test or insulin tolerance test (ITT) challenges the pituitary directly and measures its response. These tests are the gold standard for diagnosing growth hormone deficiency and adrenal insufficiency — two of the most common consequences of pituitary damage after trauma.
Step 3: Dedicated pituitary MRI.
A standard brain MRI is not the same as a pituitary MRI. A proper pituitary study uses thin-cut sequences focused on the sella turcica — the bony pocket where the gland sits. This can reveal structural changes: stalk thickening, pituitary atrophy, or small areas of tissue death that wouldn’t show on a routine scan. The medical term for this specialized imaging confirms what plain language describes — the standard scan misses it.
Timing matters. Medical guidelines recommend screening for pituitary dysfunction at 3 months and 12 months after a moderate-to-severe traumatic brain injury. Early testing can miss deficiencies that emerge as the acute phase resolves. A single normal test shortly after the crash does not close the door.
Complete a Case Evaluation form now
How Do Attorneys Prove Pituitary Gland Damage in a Truck Crash Case?
Whether filing a claim in Albemarle County with our Charlottesville car accident lawyer or navigating the courts with our Richmond truck accident lawyer, proving a pituitary injury requires the belief that we are dealing with an invisible injury. That means that we cannot show an image to a jury or insurance company of the injury. We set forth to prove this injury with the evidence that is available to us, and that evidence is often circumstantial in nature. This is where the legal work begins — and where having the right attorney matters enormously.
Here’s how we do it:
Establish the crash mechanics.
We work with accident reconstructionists and biomechanical engineers to calculate the forces involved in the specific collision — speed, angle, rotational force, change in velocity. These numbers connect the physics of the crash to the anatomy of the injury.
Document the TBI connection.
Pituitary damage follows traumatic brain injury. We build the medical record establishing that the crash caused a TBI — through emergency records, imaging, loss of consciousness documentation, and neurology evaluations. The TBI is the bridge between the crash and the pituitary.
Get the right specialist involved early.
We work with endocrinologists who have experience evaluating post-traumatic hormonal dysfunction — not just general internists running standard panels. The right specialist orders the right tests, documents the findings correctly, and can testify to causation.
Order the right imaging.
A dedicated pituitary MRI — specifically requested, with thin-cut sequences — can provide structural evidence of damage. When imaging shows stalk changes or tissue loss in a patient with hormonal deficiencies after a crash, that is objective, hard-to-dispute evidence.
Build the before-and-after picture.
We gather records from before the crash — medical history, employer records, activity levels, family testimony — to establish a clear baseline. Then we document who the person is now. That contrast is what makes damages real to a jury.
Calculate the lifetime costs.
Pituitary hormone replacement therapy — including growth hormone replacement — can cost thousands of dollars annually and continue for decades. A life care planner calculates these costs in concrete terms. Economic damages in serious pituitary injury cases can be substantial.
Retain the right experts.
These cases typically require an endocrinologist, a neuroradiologist, a life care planner, and sometimes a vocational expert. We build the expert team before the defense has a chance to define the narrative.
For more on how we handle complex medical injuries in truck crash cases, visit our Virginia truck accident lawyer page and our traumatic brain injury lawyer page. These are some of the catastrophic injuries we handle as Charlottesville personal injury lawyers.
Why Does Pituitary Gland Damage Matter in Your Case?
A pituitary gland injury is a significant injury in a personal injury case. That’s because of the severe impact these injuries can have on your quality of life, your relationships, your mental health, your ability to work, and your ability to spend time doing the things you enjoy. Medical treatment for pituitary gland injuries can be both expensive and extensive. It can require hormone replacement therapy, medications, and even surgery. This treatment can require ongoing care and it can be both invasive and difficult to manage. That makes this injury significant.
In addition, a pituitary gland injury has the following impact:
It produces objective, measurable evidence. Abnormal hormone levels and structural findings on pituitary MRI are not subjective complaints. They are documented medical findings — the kind that hold up in court.
The damages are real and long-term. Lifelong hormone replacement, ongoing endocrinology care, lost wages if you can’t return to your former work, diminished quality of life — these are significant economic damages, not just pain and suffering.
It explains the inexplicable. In cases where a victim has serious complaints but “normal” imaging, a pituitary damage diagnosis fills that gap. It gives the jury a physiological reason — rooted in the crash mechanics — for why this person is not getting better.
It is a separate injury from TBI. If you have both, you have two sets of damages. Each should be fully documented and fully compensated.
What to Do If You Think You Have Pituitary Gland Damage
- Tell your doctor specifically what you’re experiencing. Fatigue, weight changes, mood shifts, cold sensitivity, sexual dysfunction, cognitive fog. Be specific. Ask whether pituitary function has been tested.
- Request an endocrinology referral. This is not a standard emergency medicine evaluation. You may need to ask for it directly.
- Ask for a dedicated pituitary MRI. Make clear you want thin-cut imaging of the sella turcica — not just a standard brain MRI.
- Keep a symptom journal. Date, description, severity. Entries made contemporaneously are far more credible than reconstructed history.
- Do not give a recorded statement to the insurance company. Call an attorney first.
- Do not settle before this injury is identified. A settlement closes your claim. Pituitary damage diagnosed after a settlement cannot be added. The time to find this injury is before the case closes — not after.
Frequently Asked Questions
Can you have pituitary gland damage with normal scans?
Yes. Standard CT scans and even routine MRIs frequently miss pituitary damage. A dedicated pituitary MRI with thin-cut sequences is required — and even that can be normal while hormone testing shows significant deficiency. Normal imaging does not rule out this injury.
How soon after a crash does pituitary damage show up?
Sometimes immediately — but often not for weeks or months. The acute stress response of a crash temporarily elevates some hormone levels, masking deficiencies that emerge later. This is why medical guidelines recommend pituitary screening at 3 and 12 months after a serious head injury.
Is pituitary damage permanent?
It depends on the severity. Some patients recover partial or full pituitary function over time. Others have permanent deficiencies requiring lifelong hormone replacement. Growth hormone deficiency is among the most common lasting consequences.
What’s the difference between pituitary gland damage and a concussion?
A concussion is a functional brain injury — the brain’s electrical activity is disrupted. Pituitary damage is a structural and vascular injury to the hormone-producing gland. They can occur from the same crash. They require different testing and different treatment. Both can cause fatigue, cognitive problems, and mood changes — which is exactly why pituitary damage gets missed when doctors focus only on the concussion.
Can falls cause pituitary gland damage?
Yes. Serious falls — from heights, slip-and-falls with head impact, workplace falls — can generate enough force to damage the pituitary’s blood supply or stalk. Pituitary damage after a fall is well-documented in the medical literature and fully compensable in a personal injury claim.
Will I need to go to trial?
Not necessarily. Many cases resolve through settlement. But in our experience, trucking company insurers do not offer fair value on complex medical injury claims unless they know the plaintiff’s attorney is prepared to try the case. Preparation for trial is what creates settlement value.
The Bottom Line About Pituitary Gland Damage
Pituitary gland damage is one of the most overlooked consequences of serious crash injuries in Virginia. Victims are told their labs are normal. They’re told to rest. They’re told their symptoms are anxiety or depression. Meanwhile a real, physical, hormonal injury goes undiagnosed and uncompensated — sometimes for years.
At MartinWren, P.C., we handle catastrophic injury cases from truck crashes, car accidents, and serious falls throughout Virginia. As Virginia’s only Board Certified Truck Accident Attorney, I’ve spent my career building cases that require the kind of medical depth most attorneys don’t have — including injuries that don’t show up on routine imaging and don’t fit the insurance company’s playbook.
If your recovery doesn’t feel right, there may be a reason. Let’s find it together.
📞 Contact MartinWren, P.C. for a free case review
Related Brain Injury Resources:
- Vestibular Dysfunction After a Truck Crash, Car Accident, or Fall: Why “Just Dizziness” Can Mean a Serious Brain Injury
- Diffuse Axonal Injury: The “Invisible” Brain Damage That Can Occur In a Truck Accident
- Second Impact Syndrome: Why a Second Head Injury Can Be Catastrophic
- What to Expect When Pursuing a Brain Injury Claim in Virginia
- Open v. Closed Head Brain Injuries: Know the Critical Differences
Call (434) 817-3100 or complete a Case Evaluation form

